VisualEyes™ Support
Available Training
-
How to perform the Sinusoidal Harmonic Acceleration (SHA) test
-
How to perform the Velocity Step test
-
How to perform the Vestibulo-Ocular Reflex (VOR) Suppression test
-
How to use VisualEyes™ EyeSeeCam
-
How to perform the Dynamic Visual Acuity (DVA) test
-
How to perform the Advanced Dix-Hallpike test
-
How to perform the Supine Roll test
-
How to perform the Lempert (BBQ) Roll
-
How to perform the Gufoni Maneuver
-
How to perform the Epley Maneuver
-
How to perform the Dix-Hallpike test
-
How to perform the Brandt-Daroff Exercise
-
How to perform the Anterior Semont Maneuver
-
How to perform the Posterior Semont Maneuver
-
How to perform the Optokinetic Nystagmus (OKN) test
-
How to perform the Gaze test
-
How to perform the Saccade test
-
How to perform Positional Nystagmus testing
-
How to perform the Spontaneous Nystagmus test
-
How to perform the Smooth Pursuit test
-
How to perform calibration procedures
-
How to perform the Lateral Head Roll test
-
How to perform the Subjective Visual Vertical (SVV) test
-
How to perform VORTEQ™ vHIT
-
How to perform Saccadometry
-
How to perform the Active Head Rotation test
-
How to perform the Ocular Counter Roll (OCR) test
-
How to use the Research Module
-
How to perform the Gaze Stabilization Test (GST)
-
How to perform Cervical Gaze testing
-
How to perform the Functional Vision Head Impulse Test (fvHIT™)
-
How to use keyboard shortcuts in VisualEyes™
-
How to perform Pupillometry
-
How to perform Self-Paced Saccades
-
How to perform the Smooth Pursuit Neck Torsion (SPNT) test
-
How to set up and troubleshoot monitors for oculomotor and optotype tests
How to perform the Caloric test
What is the caloric test?
The caloric test is a test of the lateral semicircular canals which identifies the degree to which the vestibular system is responsive and determines how symmetric the responses are, between left and right. The caloric test does not assess vertical canal function or otolithic function.
By using caloric irrigation, you are stimulating each end organ independently of the other to determine whether one end organ is weaker than the other (asymmetry) or whether neither end organ is providing enough vestibular information to the brain.
Considerations
1. Pre-test instructions/medications
There is conflicting literature on whether you should ask patients to drop central nervous system suppressant medications for 48 hours before the VNG. Part of this debate is that patients often do not understand which medications are allowed and which are not.
A general rule of thumb is that the patient should stop taking medications that are prescribed for “dizziness” but continue to take other medications (such as heart medications, blood pressure medications, etc.).
2. Pre-test examinations
A thorough examination of the external ear canal and tympanic membrane is necessary before the caloric test. The three most important factors to consider are:
- The presence of cerumen
- The presence of a tympanic membrane (TM) perforation
- The shape of the ear canal
Presence of cerumen
If excessive cerumen is present, it might prevent the stimulus from reaching the inner-most part of the ear canal and could prohibit a reliable test result. Removal of even the smallest amounts of cerumen is beneficial to the testing process.
Presence of a TM perforation
In the presence of a TM perforation, you cannot perform caloric stimulation with water. You can only perform stimulation by air briefly to determine whether or a not a vestibular response is present. However, you cannot calculate accurate unilateral weakness and directional preponderance measures.
Shape of the ear canal
Examination of the shape and curvature of the ear canal is essential to reliable test results for two reasons:
- Because the irrigator tip is straight and ear canals rarely are, it is not uncommon for the insertion of the irrigator tip to cause slight discomfort to the patient.
- It is important that you direct the stream of air/water from the irrigator near, but not on, the tympanic membrane to avoid injury to the patient. Without a thorough examination of the ear canal, it is impossible to know whether the achieved test results are an accurate assessment of the vestibular system.
3. Vision-denied VNG
It is necessary to perform VNG with the patient in a vision-denied state to disallow fixation suppression of the nystagmus response.
4. Alerting tasks
Alerting tasks are also necessary to discourage the patient from suppressing the nystagmus. The most effective alerting tasks require the patient to use recall memory – i.e. “name a state that begins with the letter …” ,“name a color that begins with ”, “name a city in the state of ”.
5. Begin with warm irrigations
It is suggested that you begin with warm irrigations (which provide an excitatory response) if for no other reason than if the patient cannot tolerate bi-thermal irrigation, the examiner has AT LEAST enough information to provide a score for the Monothermal Warm Screening Test (MWST).
6. MWST test
MWST is a screening test used for patients who cannot tolerate bi-thermal testing. It is a percentage of asymmetry derived from only the warm-caloric irrigation.
7. Time between irrigations
You should wait between 3 and 5 minutes between irrigations, as the nystagmus from the previous test must be completely resolved before you perform the next It is suggested that you look at the eyes during the rest periods to watch the nystagmus dissipate.
Removal of the mask cover during these rest periods can be helpful to allow the patient to suppress any residual response.
8. Fixation period
A “fixation period” of 10 seconds is recommended as a diagnostic tool during the recording of the caloric response (at approximately 90 seconds after the onset of irrigation). The inability to suppress nystagmus when a fixation target is provided is considered a pathological sign of a central vestibular disorder.
Patient instructions
“I am going to put warm and cool air/water into each ear. I will begin by putting warm air in the right/left ear. The air/water will sound loud and will feel warm, but it should not be painful. If you experience pain, please tell me immediately. The air/water will be in your ear for approximately 60 seconds (30 for water). After 60 (30) seconds, I will take the air/water out of your ear and I will begin to ask you questions. I need two things from you: to keep your eyes open AT ALL TIMES – even if you are feeling 'like you are in motion' - and focus on the questions that I am asking you to answer. Do you have any questions before we begin?”
It is also helpful to reassure the patient that the sensation of motion is to be expected and will not last very long.
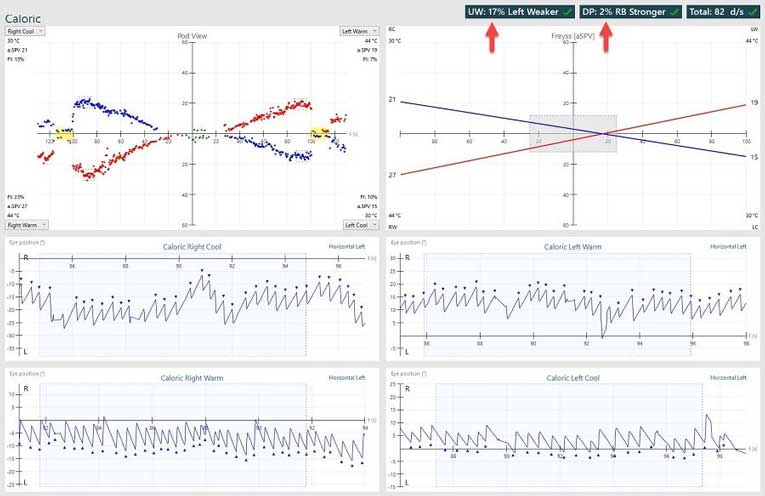
Normal caloric test results
A fully functional peripheral vestibular end organ will begin to respond to stimulation approximately 15-30 seconds into the irrigation procedure and will reach its peak approximately 60-90 seconds from the beginning of the irrigation process (air stimulus is used in the examples shown here).
A rule of thumb is that warm air/water will produce nystagmus that beats toward the test ear and cool air/water will produce nystagmus that beats away from the test ear. (COWS – Cold Opposite, Warm Same). The nystagmus beats are represented by the dots plotted on the graph for each condition. The yellow bar represents the area of maximum performance. Each condition is giving a maximum Slow Phase Velocity (SPV) value and a Fixation Index value (FI).
All 4 SPV values are added and a total SPV values is also displayed. The SPV values are used to calculate the overall weakness and to determine if any directional preponderance is present.
Common normative values for caloric response parameters
| Parameter | Labeled as | Common norm |
| Unilateral Weakness | UW% | Less than 25% |
| Directional Preponderance | DP% | Less than 30% |
| Fixation Suppression | FI% | Less than 50% |
| Bilateral Weakness | Each ear total larger than 11 degrees per second | |
| Hyperactivity | Each ear total larger than 140 degrees per second |
Threshold values for caloric testing, as referenced from Jacobson, GP, and Shepard, NT. Balance Functional Assessment and Management, 2nd Ed. San Diego; Plural Publishing, 2015
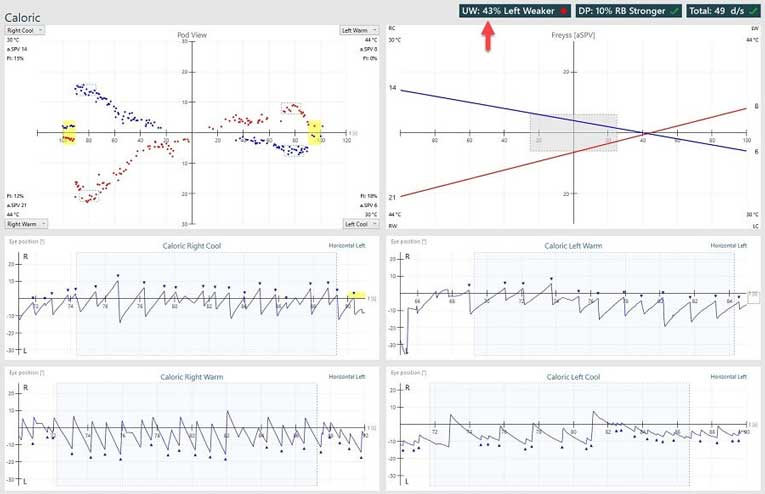
Abnormal caloric test results
Abnormal caloric test results can present in several ways: as an asymmetry between ears (labeled as “unilateral weakness”), as “directional preponderance” (“directional preponderance” numerically expresses how the amount of right-beating nystagmus compares with the amount of left-beating nystagmus) or as a display of symmetrical, but weak, responses from both ears (labeled as “bilateral weakness”).
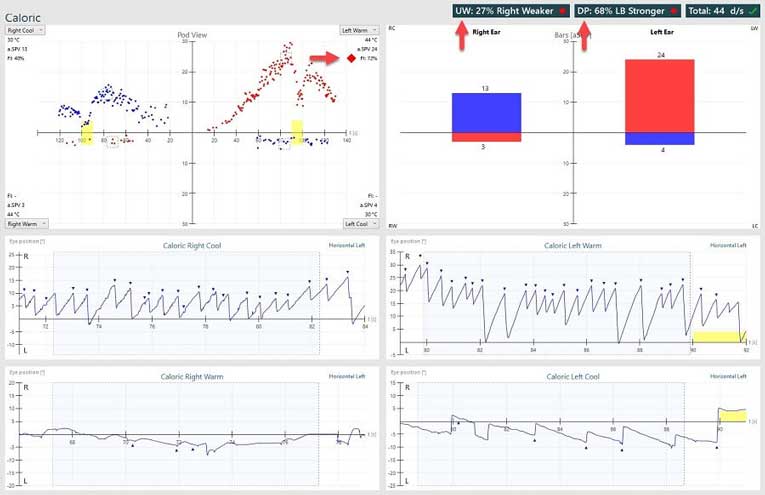
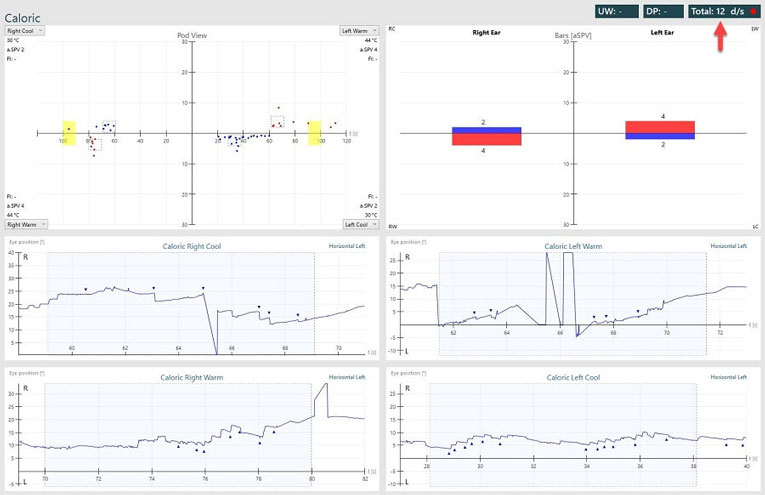
Conclusion
Caloric irrigation is the most valuable tool available to the healthcare field with which to assess vestibular function. It is the only test that allows for evaluation of each peripheral vestibular end organ independently of the other.
Caloric irrigation gives the healthcare professional an assessment of whether the peripheral vestibular end organs are functioning symmetrically and/or whether the peripheral vestibular end organs are providing the brain with enough sensory information. For a complete discussion of differential diagnosis using caloric irrigation in VNG, refer to:
Jacobson, GP, and Shepard, NT. Balance Functional Assessment and Management, 2nd Ed. San Diego; Plural Publishing, 2015
*NOTE: This is only as a guide. The patient's physician is responsible for the official diagnosis.
